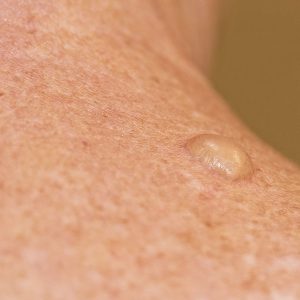
Skin Cancer & Precancerous Treatments
Skin cancer is the most common cancer, in which malignant cells are found in the outer layers of the skin. There are several different skin cancers, some of which are more threatening than others.
Skin Cancer Dermatologist & Doctor
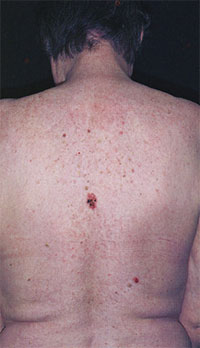 Skin cancer is the most common cancer in Portland, in which malignant cells are found in the outer layers of the skin. There are several different skin cancers, some of which are more threatening than others. It is well known that the majority of skin cancers are secondary to excessive and repeat sun exposure over an individual’s lifetime. Dermatologists thought for years that the majority of the damaging sun exposure took place prior to the age of 10. However, in the last few years this fact has been proven wrong. The majority of our sun exposure, over 80%, occurs after the age of 10. What this means is that sun protection over your whole life will decrease the risk of skin cancer.
Skin cancer is the most common cancer in Portland, in which malignant cells are found in the outer layers of the skin. There are several different skin cancers, some of which are more threatening than others. It is well known that the majority of skin cancers are secondary to excessive and repeat sun exposure over an individual’s lifetime. Dermatologists thought for years that the majority of the damaging sun exposure took place prior to the age of 10. However, in the last few years this fact has been proven wrong. The majority of our sun exposure, over 80%, occurs after the age of 10. What this means is that sun protection over your whole life will decrease the risk of skin cancer.
According to the American Cancer Society, Skin cancer is the most common of all cancers. It accounts for nearly half of all cancers in the United States. More than 3.5 million cases of basal and squamous cell skin cancer are diagnosed in this country each year. Melanoma, the most serious type of skin cancer, will account for more than 76,600 cases of skin cancer in 2013.
The Three Most Common Types of Skin Cancer Are
- Basal Cell Carcinoma (76%)
- Squamous Cell Carcinoma (20%)
- Melanoma (4%)
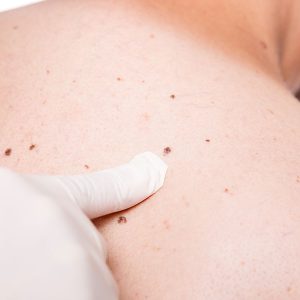
Take your clothes off and do regular self-examinations; look for new moles and moles that are changing. Look for the mole or growth that looks like it does not belong on you.
What Does Skin Cancer Look Like?
Skin cancer may start as a new growth, a sore that does not heal or a change in the appearance of a mole or freckle. Skin cancers look different from one another. It is important look for skin cancer signs by knowing what your moles currently look like to be able to tell if they have changed and become cancerous. Skin cancers are generally found on areas of the skin that are exposed to the sun, including the head, neck, face, hands and arms.
Basal Cell Carcinoma
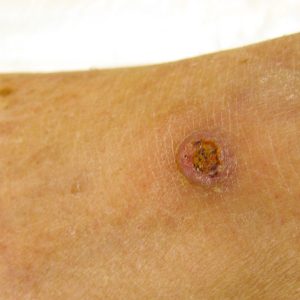
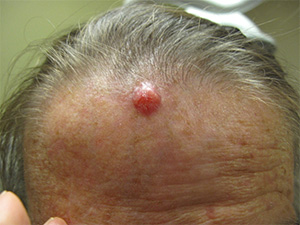 Basal cell carcinoma (BCC) is the most common type of skin cancer. In most cases it appears on skin that gets a lot of sun, such as the face, scalp, neck, hands, and arms. Basal cell carcinoma generally is a skin bump or growth that is pearly or waxy and is normally flesh colored or light pink.
Basal cell carcinoma (BCC) is the most common type of skin cancer. In most cases it appears on skin that gets a lot of sun, such as the face, scalp, neck, hands, and arms. Basal cell carcinoma generally is a skin bump or growth that is pearly or waxy and is normally flesh colored or light pink.
Basal skin cancer grows slowly and usually does not spread to other parts of the body. But it should still be treated promptly. Treatment of basal cell skin cancer varies depending on the size, depth and location of the lesion.
Squamous Cell Carcinoma
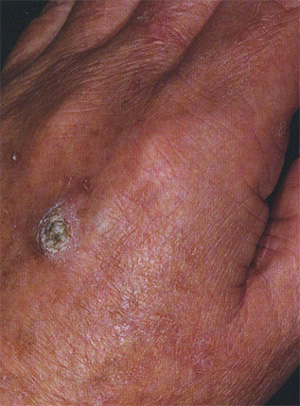 Squamous cell carcinoma (SCC) is the second most common type of skin cancer and accounts for approximately 25% of all skin cancers. This form of skin cancer arises in the squamous cells that make up most of the skin’s upper layers (epidermis).
Squamous cell carcinoma (SCC) is the second most common type of skin cancer and accounts for approximately 25% of all skin cancers. This form of skin cancer arises in the squamous cells that make up most of the skin’s upper layers (epidermis).
It tends to form on skin that gets frequent sun exposure including the rim of the ear, face, neck and arms. Anyone who has had a basal cell carcinoma is also more likely to develop squamous skin cancer. This skin cancer looks like a firm bump, scaly patch or an ulcer that heals and then re-opens, and is usually red in color. Squamous Cell Carcinoma may even look like a wart and sometimes appear as open sores with a raised border and a crusted surface. Squamous cell carcinomas detected at an early stage and removed promptly are usually curable and cause minimal damage.
However, left untreated, they eventually penetrate the underlying tissues and can become disfiguring. Squamous cell carcinoma also has a low risk of metastasis. Treatment of squamous cell carcinoma varies depending on the size, depth and location of the lesion: C & D, excision and MOHS surgery.
Melanoma
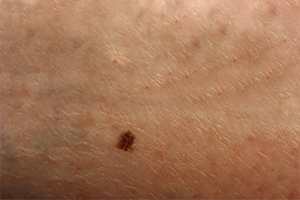 Melanoma is the most serious form of skin cancer. If it is caught and treated early, it is almost always curable. Seeking the help of an experienced dermatologist in Portland is always a great way to ensure you’re getting the help that you need. However, if it is not caught early on it becomes hard to treat and can be fatal. Fair-skinned individuals with light hair and eye color have an increased risk of developing melanoma. Additionally, those who have a family history of the disease or have ever had skin melanoma or other skin cancer are at greater risk.
Melanoma is the most serious form of skin cancer. If it is caught and treated early, it is almost always curable. Seeking the help of an experienced dermatologist in Portland is always a great way to ensure you’re getting the help that you need. However, if it is not caught early on it becomes hard to treat and can be fatal. Fair-skinned individuals with light hair and eye color have an increased risk of developing melanoma. Additionally, those who have a family history of the disease or have ever had skin melanoma or other skin cancer are at greater risk.
This skin cancer generally appears suddenly as a new dark spot or may be a mole that is changing. Moles that are asymmetric, irregular with multiple colors and the size of a pencil eraser may be worrisome for melanoma. In addition growths that change noticeably in size or have irregularities in shape and color could be melanomas. It is important to check your skin from head to toe regularly for lesions that have the ABCDEs of melanoma symptoms.
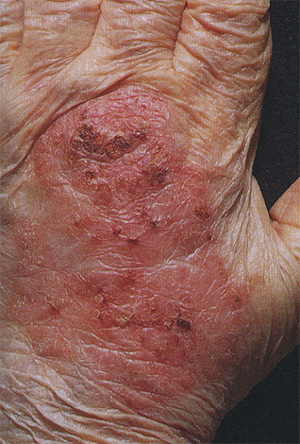
ABCDE of Melanoma:
A = Asymmetrical (one side is not the mirror of the other)
B = Border is irregular (not oval or circular)
C = Colors are multiple (red, brown, tan, black)
D = Diameter is larger than 6mm (pencil eraser size)
E = Evolving and changing over time for a new or an old mole.
See Mole Mapping
Skin Cancer Treatment in Portland
Curettage and Electrodessication (C & D) for Skin Cancer
The skin cancer is scraped off with a scalpel and a curette. The procedure is repeated a three times to ensure that all cancer cells are removed. C & D has almost the same cure rate as excising or cutting out the skin cancer.
Excisional Surgery for Skin Cancer
Removal of the entire skin cancer along with a surrounding border of apparently normal skin. The typical “normal skin” margin is around 5mm. The incision is closed with sutures and the growth is sent to the lab to verify that all the cancerous cells were removed. MOHS surgery is a surgical treatment that is used to treat skin cancers on the face.
Skin Cancer Prevention in Portland
 Most skin cancers result from too much sun (UVA and UVB) exposure. The ultraviolet A (UVA) rays can cause premature wrinkling, brown age spots while the ultraviolet B (UVB) rays cause sunburns. Both types of radiation, UVA and UVB, are harmful and can cause skin cancer. It is essential to protect your skin from these damaging rays in order to prevent skin cancer. Not only do sunburns increase skin cancer, a tan is a sign of sun damage and will increase your risk of skin cancer.
Most skin cancers result from too much sun (UVA and UVB) exposure. The ultraviolet A (UVA) rays can cause premature wrinkling, brown age spots while the ultraviolet B (UVB) rays cause sunburns. Both types of radiation, UVA and UVB, are harmful and can cause skin cancer. It is essential to protect your skin from these damaging rays in order to prevent skin cancer. Not only do sunburns increase skin cancer, a tan is a sign of sun damage and will increase your risk of skin cancer.
Sun Protection
Sun protection includes sunscreen but more importantly wearing a hat, sunglasses, protective clothing and looking for shade to avoid the sun are the best sun protection measures. Every day you should be applying a broad-spectrum sunscreen with a Sun Protection Factor (SPF) of 30 to your face. New FDA rules require sunscreen manufactures to have both a UVA and UVB sunscreen in their product.
Annual Skin Checks:
 It is important to do self-examinations and become with your skin and the pattern of your moles. Also, get annual skin checks especially if you have a personal history or a family history of skin cancer, multiple sunburns and/or very fair skin. Mole mapping may be helpful in monitoring your moles.
It is important to do self-examinations and become with your skin and the pattern of your moles. Also, get annual skin checks especially if you have a personal history or a family history of skin cancer, multiple sunburns and/or very fair skin. Mole mapping may be helpful in monitoring your moles.
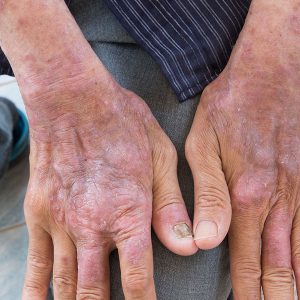
Actinic Keratosis (Pre Skin Cancer)
Actinic keratosis (AK) is the most common type of precancerous skin lesion. An actinic keratosis is evidence that sun damage has occurred and that the individual is at greater risk of developing skin cancer. Actinic keratosis normally occur on the skin that has had the most sun damage like the face, lips, ears, scalp, neck, back of the hands, shoulders, forearms and back. When an actinic keratosis develops on the lip, they are called Actinic Cheilitis. Actinic keratosis usually appear as small crusty, scaly bumps ranging in size from 1 mm to 1 inch. They are dry and rough to the touch and can be raw or sensitive. If actinic keratosis are treated early, they can almost always be completely removed before turning into skin cancer. However, if left untreated, actinic keratosis may develop into squamous cell carcinoma.
Precancerous Skin Treatment
Cryotherapy
Liquid nitrogen is applied to the lesion to freeze it off.
Photodynamic Therapy (PDT)
A topical agent, Levulan, is applied to the pre-skin cancer (AK’s) and the skin around it for 1 – 2 hours the treated skin is exposed to Blu light that activates the Levulan and selectively destroys AKs while causing minimal damage to the surrounding skin.
Topical Chemotherapy Agents
These treat both visible and invisible lesions with minimal risk of scarring. Common topical agents include Imiquimod and Fluorouracil. Imiquimod is called a biologic agent because it turns up the patient’s own immune system to fight off the cancer and pre-cancer cells. Imiquimod was first introduced to treat skin cancers in the late 1990’s. Imiquimod treats both actinic keratosis and superficial basal cell skin cancer and superficial squamous cell skin cancer. The cure rates for this treatment are not as high as excisions or MOHS surgery, though. Fluorouracil is a chemotherapy treatment that targets cancer cells and kills them. Fluorouracil has been around for decades and is very useful for treating pre-skin cancers.
Imiquimod
Pre-cancers and cancerous lesions of the skin are usually treated with either surgical methods or liquid nitrogen. A topical cream, Imiquimod, has been on the mark for over 15 years to treat these lesions. Imiquimod is a cream that when applied to the precancerous lesions, increases the body’s own immune system to fight the abnormal cells. This process provides you a non-surgical option to treat the cancer and/or pre-cancerous cells. Imiquimod cream is FDA approved to treat superficial Basal Cell Carcinoma, Actinic keratosis, as well as squamous cell carcinoma and even malignant melanomas.
Treatment for pre-cancers (actinic keratosis) may be 6 – 8 weeks and 12-16 weeks for basal cell skin cancer.
Application instruction Note – packets are very tiny and may be used multiple times.
- Open the packet with scissors or a simple pinhole. Gently squeeze the pouch and with a toothpick, remove a tiny amount of cream to cover the area you wish to treat.
- Place the small amount of cream on the center of the area to treat.
- Do NOT spread the cream to the surrounding tissue as this may cause unnecessary irritation.
- Apply the Imiquimod cream three times a week to start – usually Monday, Wednesday and Friday. Stop application when a rash or redness develops at the site of application. Wait for 10 days until the redness or rash clears, then restart the Imiquimod cream. Continue starting and stopping the Imiquimod as directed for a total of 12 weeks.
After each application fold the packet over and store it in a plastic baggy. Ignore the “single application” labeling.
Imiquimod Treatment Reactions
After 2-4 applications the skin may become red and scaly, heaped up and crusty or weepy and crusty. This is an anticipated side effect. If your skin becomes too irritated from the product, stop product application and apply Polysporin or Bacitracin 2-3 times a day for 3-4 days after soaking the crusts with some plain warm water for 5 minutes. Once the reaction response has been minimized, begin with the Imiquimod again but less frequently, maybe once or twice a week. I f no reaction occurs, increase to 5 days for a week, then daily for a week. Some people do not react at all. On occasion one can get a very big aggressive inflammatory reaction with extensive crusting. This response does fade after discontinuation of product and any residual skin changes will fade.
Expected Results
At the end of treatment the skin in the pre-cancerous areas usually looks smooth and soft. In the areas where you have had cancer it may be white and there may be some scarring. If the cancer was large enough to destroy tissue, there may be a depression left behind. It does take at least 3-4 months for color changes to blend with the rest of the skin and there may be areas of blotchy pigmentation where the color is just not quite even. The cosmetic results are generally better than surgery; however, further treatment may be needed for deeper lesions before using Imiquimod.
You can learn more about skin cancer & pre-cancer treatments at American Academy of Dermatology.