Portland Eczema Treatments
Atopic Dermatitis which is also known as eczema is a common itchy skin disease that typically starts early in infancy or childhood.
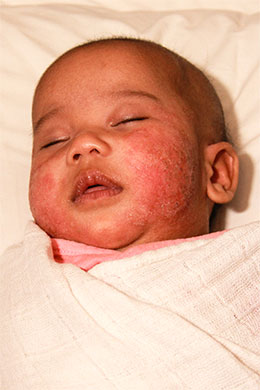 What is Eczema (Atopic Dermatitis)?
What is Eczema (Atopic Dermatitis)?
Atopic Dermatitis which is also known as eczema is a common itchy skin disease in Portland that typically starts early in infancy or childhood. It affects approximately 17% of children and usually begins in the first year of life. The symptoms include intense itching along with red scaly lesions. Most children grow out eczema.
We are learning more about the cause of eczema each year. Recently it was found that many patients with Atopic Dermatitis have a mutation in a gene that produces a protein called fillagrin. Fillagrin is necessary for the barrier of our skin to be intact and protecting. The defect leads to immune/inflammatory dysregulation. What this means is that environmental triggers, dry skin, skin infections will all be potential triggers for flaring and worsening the eruption. In addition we know there is a genetic predisposition for patients to develop eczema. If a first-degree family member has either eczema, hayfever or asthma an individual is predisposed to get any one of those three (eczema, hayfever or asthma.) Food allergies rarely play a role as the cause of eczema.
So, throughout the life of someone with eczema there is an increased risk of developing both hayfever and/or asthma. Unfortunately, many children maintain hyperirritable, dry, itchy and rashy skin well beyond childhood with flares that come and go.
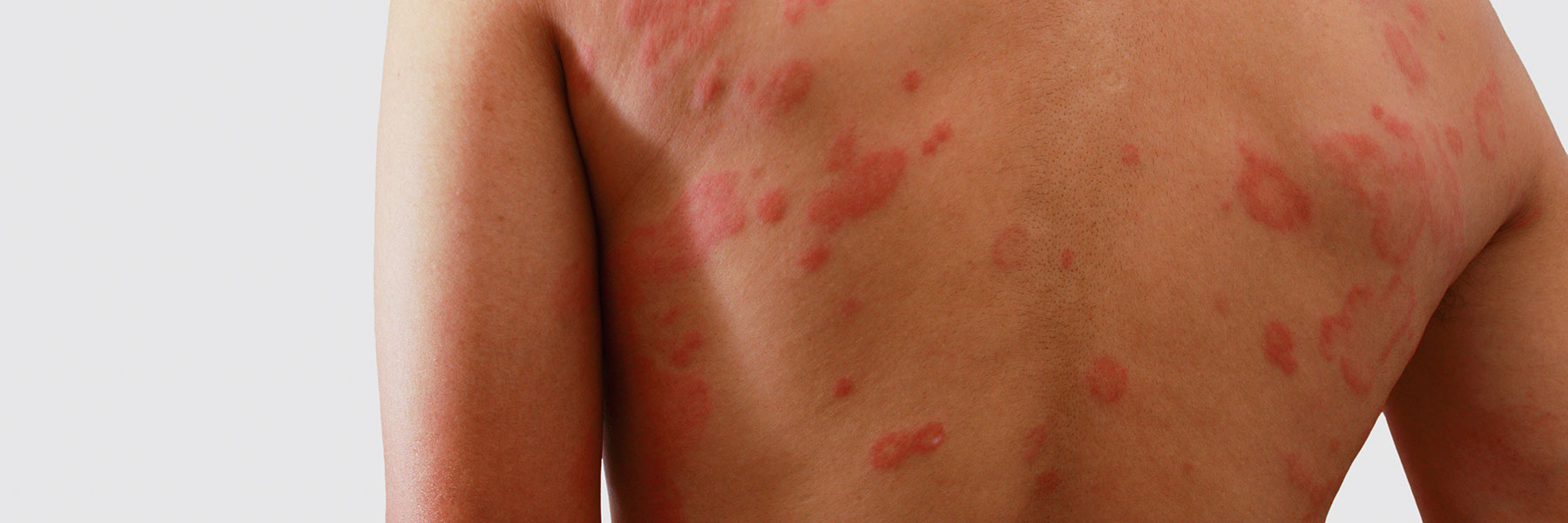
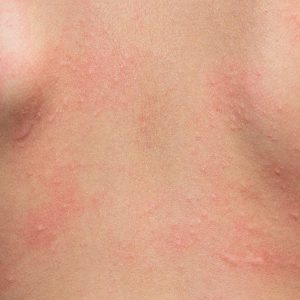
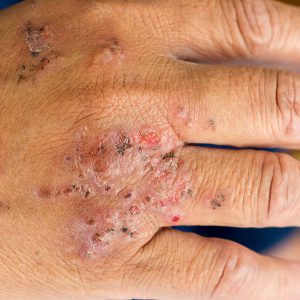
What Does Eczema Look Like?
The rash in eczema involves predictable areas of the body depending on age. In infancy the rash affects the face and the extensors of the lower legs. In childhood, the flexural surfaces of the skin are involved (behind the knees and in the creases of the elbows).
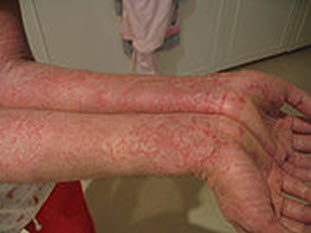 In adults the rash is more diffuse and is commonly on the eyelids, necks, stomach, belly button, and extremities. Patients with eczema also have other conditions: follicular red scaly bumps on the back of the arms and sometimes thighs (keratosis pilaris), increased lines on the palms of the hands, a little fold under the eyelid (Denny Morgan folds), dry scaly skin.
In adults the rash is more diffuse and is commonly on the eyelids, necks, stomach, belly button, and extremities. Patients with eczema also have other conditions: follicular red scaly bumps on the back of the arms and sometimes thighs (keratosis pilaris), increased lines on the palms of the hands, a little fold under the eyelid (Denny Morgan folds), dry scaly skin.
There are several other skin eruptions that may look like Atopic Dermatitis: allergic contact dermatitis (allergy to something that is touching the skin – like poison oak, metals, topical antibiotics, moisturizers), seborrheic dermatitis (dandruff on the scalp, face and chest), scabies, tinea corporis (ring worm), psoriasis, immunodeficiency (rare), molluscum dermatitis (viral infection with small wart like flesh colored papules – common in children). These other skin eruptions need to be ruled out to help direct the most appropriate treatment.
What Causes Eczema?
Eczema Treatment
Hydrate the Skin
Hydration of the skin is essential. WATER is good for the skin if it is trapped in with a moisturizer. WATER is bad for the skin if it is allowed to evaporate off the skin after bathing. Bath in a warm water bath for 20-30 minutes once or twice a day (until the fingertips are wrinkled and prune like) followed by immediate application of a greasy moisturizer. Ointments are the best moisturizers because they trap the water on the upper layer of the skin in and hold it there for much longer than a lotion or cream. Lotions and creams have a lot more water in them that does not rub in, but evaporates off the skin and actually may cause more dryness. In addition creams and lotions have more chemicals in them that may potentially become allergens. We understand that ointments are greasy and messy. So – if a cream must be used with recommend: CeraVe Cream, Vanicream and Cetaphil Cream. In addition when bathing minimizing soap is a good idea. Soaps that are good are pH balanced: Cetaphil, Vanicream, Unscented Dove. Avoid soaps and bubble bath. Soaps like Ivory and Baby Shampoo products are very irritating to the skin.
Avoid Irritants
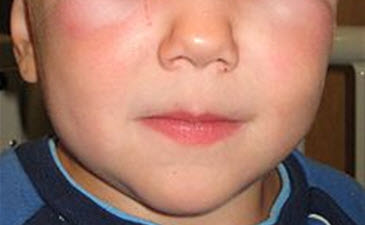
Irritants on the skin may worsen eczema. The best example of an irritant is WATER. As mentioned above water trapped into the skin with a greasy moisturizer is very good for patients with eczema. But chronic wetting and drying of the skin from drool on a baby’s face will lead to facial rash in a baby with eczema. In addition, even contact with food and saturated wet bibs around the neck may lead to a rash around the mouth, neck and chest. Applying a thick moisturizer barrier (like Vaseline) before mealtime and after mealtime may prevent this.
Environmental Factors
Other factors that may flare the skin include seasonal allergies, upper respiratory illness, bacterial infection, pollution and vaccinations. If the patient has itchy, runny eyes and rubs the skin, the rash of Atopic Dermatitis will develop – from scratching and rubbing itchy skin.
Topical Treatment for Eczema
Topical steroids are first line treatment for Atopic Dermatitis. Hydrocortisone 1% is the weakest steroid and does not require a prescription. It is safe to use on the face and in the thinned skin areas – such as the creases of the arms, behind the knees and on the neck. Triamcinolone 0.1% ointment is often used to treat the rash below the neck on the trunk, hands and feet. The STRENGTH of the steroid is NOT based on the % number on the label. Steroids classes use different numbering systems. For example Hydrocortisone is 1% and Triamcinolone is 0.1%. Triamcinolone is stronger. We recommend that active flares are treated aggressively one or twice a day for 2 weeks. The steroid should then be decreased to every other day and then every third day. Overuse of steroids can lead to thinning of the skin; change the texture of the skin (feeling like cigarette paper), stretch marks as well as the formation of lighter and darker pigmented spots. RULE OF THUMB: if the area of skin does not itch – do not treat!
Tacrolimus: Protopic or Elidel are Second Line Treatments
Tacrolimus (Protopic) is calcineurin inhibitors. It is NOT a steroid. It is approved for use in children over the age of 2. Tacrolimus works like a steroid by decreasing inflammation associated with eczema. Tacrolimus is a wonderful alternative because it is greasy so it traps in moisture and it is safe to use on the face and think skin areas, where side effects of topical steroids are the greatest. Tacrolimus does not have the side effects of steroids. The FDA put a black box warning on the calcineurin inhibitors worrying about potential for cancer. This warning is being fought by the Academy of Dermatology with hopes it will be removed in the upcoming year. Tacrolimus may cause stinging, but this does not mean it is causing an allergy. This is a common side effect that sometimes can be stopped by refrigerating the medication.
Treat Superficial Skin Infections
Patients in Portland with eczema are commonly infected with superficial skin bacteria like staphylococcus aureus. The infection presents as white pus bumps or a yellow and crusted rash that looks different from the eczema. The infection may actually cause the skin to flare more and will continue to flare until the infection is treated. Many patients are “carriers’ of Staphylococcal aureus. This means you carry or harbor the bacteria in places like the nose, crack of buttocks and belly button. Being a carrier means the bacteria is not causing an infection in these areas. But, since you carry the bacteria on the skin it can be moved to other more vulnerable areas where the eczema rash is flaring.
Decolonize
To clear the “carrier state” we recommend treating with Mupirocin 2 times a day for 7 days, then STOP. Do not over use Mupirocin or resistance will develop to the bacteria. In addition we recommend BLEACH BATHS to decrease the overall bacteria on the skin. A bleach bath is similar to swimming in a pool! ¼ cup of bleach is put in a full bath 2 times a week. The treatment will keep the overall bacteria on the skin down without creating resistance to the bacteria. Overuse of antibacterial soaps has increased the number of resistant bacterial strains. NOTE: SIMPLE COLD SORES: may cause a severe type of eczema called: ECZEMA HERPETICUM. This is severe and requires immediate medical attention. Careful treatment of cold sores in the patient and family members helps prevent this problem.
Antihistamines May Help You Sleep
Antihistamines: Benadryl, loratidine, Allegra, Zyrtec. There is LITTLE evidence to support that antihistamines actually help with itching in Atopic Dermatitis. But, sleep loss is the result of severe itching and is a significant problem in Atopic Dermatitis. A sedating antihistamine at bedtime (Benadryl, Hydroxyzine or Doxepin) may help with sleep and decrease the itch. If the patient has hayfever symptoms in addition to eczema, a non-sedating antihistamine like loratidine may be helpful. The dose is 5mg a day for ages 5 and under and 10mg a day for ages 6 and older. Allegra dosing is 60mg two times a day or 180mg once a day and Zyrtec 10mg once a day.
Oral Medications
Prednisone suppresses the inflammation associated with eczema and may be prescribed in a two to three week taper (1-2mg/kg/day). Using topical treatment at the same time will decrease the chance of a rebound flare (the dermatitis coming right back when finished with the prednisone). Prednisone has many side effects, so long term use is not recommended. In addition to prednisone other systemic drugs are used to treat severe eczema including Methotrexate, Cyclosporine, and the newer biologic medications like Enbrel.
Light Treatment
Narrow band UVB is a therapeutic wavelength of light that is given in the office 2 or 3 times a week. Light treatments can help clear Atopic Dermatitis by decreasing inflammation. Mid day sun may also be helpful in clearing the eruption. Patients tend to do better over all during the summer months because of the effects of sunlight.
Role of Allergy in Eczema (Atopic Dermatitis)
First and foremost focus on treatment of eczema or atopic dermatitis is good skin care. Allergic reactions to foods or to topical products are RARELY the cause of eczema. Diet restrictions frequently do not change the course of the dermatitis. Foods may cause direct skin contact irritation when the food touches the skin while eating. Applying protective barriers before eating, such as Vaseline will help this.
Hives and Eczema are Different
 Looking for a food allergy can detract from focusing on good skin care in an Atopic patient. IgE mediated (immunologic – antibody driven allergic reactions to foods like nuts and seafood is common in Atopic patients (up to 1/3).
Looking for a food allergy can detract from focusing on good skin care in an Atopic patient. IgE mediated (immunologic – antibody driven allergic reactions to foods like nuts and seafood is common in Atopic patients (up to 1/3).
These eruptions do not cause eczema. Most patient’s allergy to nuts will develop hives, swelling of the lips and even breathing difficulties or anaphylaxis. Prick testing has been shown to poorly predict clinical reactions in Atopic dermatitis. IMPORTANT NOTE: An indirect relationship between food allergies and eczema does exist. Allergies to foods may lead to more itching and scratching of the skin, which may worsen or FLARE the eczematous eruption.
Food Induced Eruptions are Rare
Food induced Atopic dermatitis is rare. A “Rare foods diet’ is required to determine if foods are causing or worsening the dermatitis. This is done over the course of weeks. First the patient discontinues antihistamines for at least one week prior to the testing. Initially the diet is restricted to lamb, turkey and rice. These are foods that are rarely consumed and rarely allergenic. At each meal add in at least 30 gm. of the critical food group, one at a time: milk, wheat, egg, soy etc. Then important foods are added; chicken, pork, beef, green vegetables, and potatoes, citrus. And, finally other suspected foods (foods commonly consumed in the diet). For the two hours after eating watch for signs of itching or inflammation (redness, swelling scaling of skin). If a reaction occurs – make a note and a rechallenge should be done 1 to 2 days later to confirm the reaction. Seafood’s and nuts are associated with anaphylactic and hive like reactions and are excluded from testing.
Environmental Allergens Like Dust Mites
Reduction of house dust mite in a small pediatric may improve Atopic Dermatitis symptoms. Frequent hot water washing of sheets, pillowcases and blankets; vacuuming carpets, upholstery may help. Replace carpet with linoleum, tile or hardwood helps decrease dust mites.
Stress May be a Trigger for Eczema Flares
Trying to lower stress though relaxation therapy, massage, hypnotherapy, psychotherapy, and exercise may all improve the well being of the patient with Atopic Dermatitis. Stress has been shown to alter immune cell function and neuroendocrine effects. It may also alter the skin barrier state.
You can learn more about eczema (Atopic Dermatitis) at American Academy of Dermatology.